Dynamics of language recovery in post-stroke aphasia: A longitudinal neuroimaging study
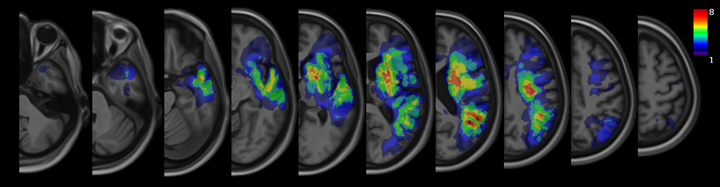 Lesion overlap in 19 post-stroke subjects
Lesion overlap in 19 post-stroke subjects
Language impairments (also known as aphasia) represent a common side effect of stroke, affecting one in three survivors. Although aphasia does not affect the intelligence of an individual, it alters the way someone speaks, understands, reads, or writes.
Here are some examples of the frustrations encountered by patients and their caregivers regarding stroke-induced aphasia: “I get frustrated when people can’t understand me”; “We continually struggle to get medical professionals to recognize that he is not stupid when he gets treatment. He is ignored when he tries to communicate”; “One of the worst effects on my son is the loss of friends, workmates and his freedom. He cannot converse with his friends now” (from the Life After Stroke Campaign Report – Summer 2013).
The loss of the ability to communicate dramatically affects the daily life and well being of patients and their caregivers. Some patients spontaneously recover their language symptoms over time but to this date, we still do not know which changes in the brain favor this improvement.
Our project provides a unique opportunity to study the brain mechanisms that support language improvement in post-stroke aphasia in a longitudinal perspective (<3 days, 10-14 days, 6 months), by combining detailed language evaluations and images of their brain using Magnetic Resonance Imaging. More specifically, sophisticated protocols of brain image analysis will be used allowing us to study the fibers connecting different brain regions.
Understanding the brain changes associated with the improvement of language symptoms will enable: 1. the development of new treatments that will enhance or accelerate these changes and 2. the implementation of new scientifically-based early intervention protocols to be administered as part of the clinical routine in acute care facilities.
Ultimately, this line of research will enable the optimization of intervention therapies and the maximization of communication outcomes in aphasic patients.
Collaborators
- Dr Karine Marcotte, Montréal
- Dr Alex Desautels, Montréal
- Dr Maxime Descoteaux, Sherbrooke
Postdoctoral fellows working on this project
Students working on this project
- Johémie Boucher
- Mariem Boukadi
- Amélie Brisebois (co-dir)
- Alberto Osa (co-dir)